As we learn more about the pathophysiology of diabetes mellitus, we find that there is more yet to be discovered. Diabetes mellitus is a syndrome with disordered metabolism and inappropriate hyperglycemia due to either a deficiency of insulin secretion or to a combination of insulin resistance and inadequate insulin secretion to compensate. Type 1 diabetes is due to pancreatic islet B cell destruction predominantly by an autoimmune process, and these persons are prone to ketoacidosis. While type 2 diabetes is the more prevalent form and results from insulin resistance with a defect in compensatory insulin secretion. Diabetes can lead to serious complications, resulting in multiple diseases or disorders that affect multiple systems that may result in premature death.
Normal Pathology of the Human Body
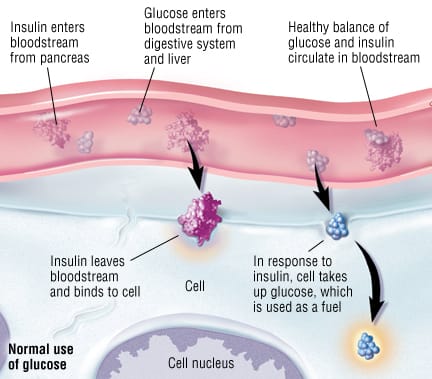
In people that are healthy, the pancreas, an organ located behind the liver and stomach, secretes digestive enzymes and the hormones insulin and glucagon into the bloodstream to control the amount of glucose in the body. The release of insulin into the blood lowers the level of blood glucose (simple sugars from food) by allowing glucose to enter the body cells, where it is metabolized. If blood glucose levels get too low, the pancreas secretes glucagon to stimulate the release of glucose from the liver. Right after a meal, glucose and amino acids are absorbed directly into the bloodstream, and blood glucose levels rise sharply. The rise in blood glucose levels signals important cells in the pancreas, called beta cells, to secrete insulin, which pours into the bloodstream. Within 20 minutes after a meal insulin rises to its peak level.
Insulin enables glucose to enter cells in the body, particularly muscle and liver cells. Here, insulin and other hormones direct whether glucose will be burned for energy or stored for future use. When insulin levels are high, the liver stops producing glucose and stores it in other forms until the body needs it again. As blood glucose levels reach their peak, the pancreas reduces the production of insulin (about 2 - 4 hours after a meal both blood glucose and insulin are at low levels).
Type 1 Diabetes
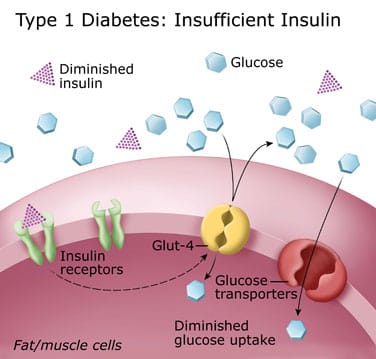
Type 1 diabetes is usually diagnosed in children and young adults. It develops when the body’s immune system destroys pancreatic beta cells, the only cells in the body that make the hormone insulin, which regulates blood glucose.
Only 5% of people with diabetes have this form of the disease. To survive, people with type 1 diabetes must have insulin delivered by injection or a pump.
Type 2 Diabetes
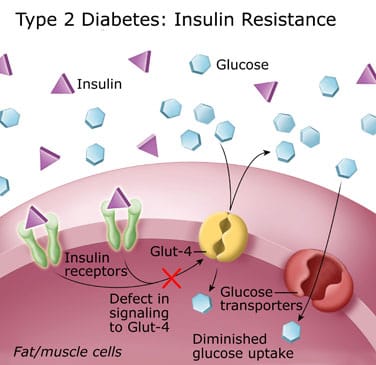
Type 2 diabetes is the most common form of diabetes. The causes of type 2 diabetes are multi-factorial and include both genetic and environmental elements that affect beta-cell function and tissue (muscle, liver, adipose tissue, and pancreas) insulin sensitivity. In type 2 diabetes, either the body does not produce enough insulin or the cells ignore the insulin. It usually begins as insulin resistance, a disorder in which the cells do not use insulin properly. As the need for insulin rises, the pancreas gradually loses its ability to produce it.
When glucose builds up in the blood instead of going into cells, it can cause far-reaching health implications like heart disease, nerve damage and kidney damage. Diabetes is the leading cause of kidney failure, non-traumatic lower-limb amputations, and new cases of blindness among adults in the United States.
You can prevent or delay the onset of type 2 diabetes through a healthy lifestyle such as changing your diet, increasing your level of physical activity, maintaining a healthy weight... with these positive steps, you can stay healthier longer and reduce your risk of diabetes.