Choosing the care path for critically ill patients is essential to achieving optimal outcomes for both patients and providers. For patients, without the right clinical capabilities and surrounding environment in which to recover, they may suffer medical setbacks that impede recovery. For providers, such as hospitals, major penalties (including extensive fines) can be incurred due to patients readmitting after discharge.
All of these considerations make knowing when and where to discharge high acuity patients a challenging and unique, case-by-case process.
In this whitepaper, we outline the clinical capabilities that distinguish two post-acute care (PAC) settings and assess the most appropriate patient types for each to help deliver better results for chronically, critically ill patients and providers alike.
Benefits of Long-Term Acute Care (LTAC) Hospitals: Complex, Intensive Care
Long-term acute care hospitals are in a unique position to effectively treat
critically ill patients. Unlike other post-acute settings, long-term acute
care hospitals can help patients who need to see a physician or several
specialty physicians every day. These specialists coordinate care with an
interdisciplinary team made up of nurses, therapists, dietitians, pharmacists
and other specialists.
These experts work together to determine the best treatment options and care plan for each and every patient. Most treatment plans involve many clinical disciplines, are complex, intensive, and evolving, and may require a length of stay measured in weeks.
Long-term acute care hospitals have three key benefits:
- They have the same licensing, accreditation, and certification standards as traditional hospitals, yet offer the personalized focus of a smaller hospital.
- Government data shows that this type of care can reduce hospital readmissions by 26-44%.1
- As an acute-care hospital, LTAC hospitals costs per-patient-day are generally 25-34% lower than traditional hospitals.2
A Growing Need for LTAC Hospitals
America’s aging population is now suffering from far more chronic and critical illnesses, and the trend is only worsening. By 2030, about 40% of people aged 65 and older will suffer from three or more chronic conditions.3 This is creating a surge in demand for PAC facilities that are able to successfully treat these seriously ill patients.

Compounding this need is the recent pressure from the Centers for Medicare and Medicaid Services to decrease rehospitalizations. CMS is bolstering their value-based purchasing program, which reduces payments to providers with overly high readmission rates.4 These shifts in legislation and the associated penalties are pushing providers to strive for the best possible patient outcomes and to choose post-acute care treatment settings that are the most clinically effective.
While LTAC hospitals provide care for a very high-acuity, niche patient population, they play a vital role in achieving more efficient recovery of patients who have a high risk of readmission due to their clinical complexity. By transitioning these challenging patients to a LTAC hospital, when it is the most appropriate site of care for their needs, a significant portion of financial losses for short-term providers can be avoided.
LTAC Hospital Expertise in Pulmonary Patients
LTAC hospitals are in a unique position to care for complex pulmonary patients because they provide acute-level care to critically ill patients, with a particular competency for those with pulmonary issues. Further, many pulmonary patients have multiple comorbidities, meaning they would benefit from seeing a physician or several specialty physicians every day, something LTAC hospitals offer. To aid in this pulmonary expertise, most LTAC hospitals offer 24/7 respiratory coverage. It is important for providers and physicians to identify post-acute partners who can provide expert care for complex pulmonary patients to help reduce readmissions and avoid penalties.
Differences between SNFs and LTACHs:
Skilled Nursing Facilities are often an appropriate setting for patients who have extended medical needs that cannot be cared for in a lower level of care, such as at home. These facilities are most suitable for patients who are not in a critical stage of illness as they offer physician or physician–extended visits on a weekly or as-needed basis.
SNFs are most appropriate for patients, often medically stable, who require 24-hour nursing care and an interdisciplinary approach to care delivered by therapy and nursing staff, rather than a team of physicians. Super SNFs are nursing centers with expanded capabilities, able to accommodate more clinically-complex patients.5 Nevertheless, they remain focused on providing therapies to patients who are no longer critical and are ready to begin a rehab program, so the same key clinical elements of comprehensive acute-level care offered in LTAC hospital are not as readily available.
With more and more of the older population interested in aging at home, many SNFs are attempting to grow beyond their conventional offerings. SNFs around the country are exploring options like palliative care, expanded residential accommodations, and addiction recovery services to better connect with a larger patient demographic.

What About Super SNFs?
Super SNFs are nursing centers with expanded capabilities, able to accommodate more clinically-complex patients.5 These facilities are equipped with specialists and advanced medical technologies not generally available in a standard SNF. Nevertheless, they remain focused on providing therapies to patients who are no longer critical and are ready to begin a rehab program, so the same key clinical elements of comprehensive acute-level care offered in LTAC hospital are not as readily available.
Comparing Levels of Care
To better understand the levels of care offered by different types of post-acute facilities, refer to this comparison chart:
Expand Chart
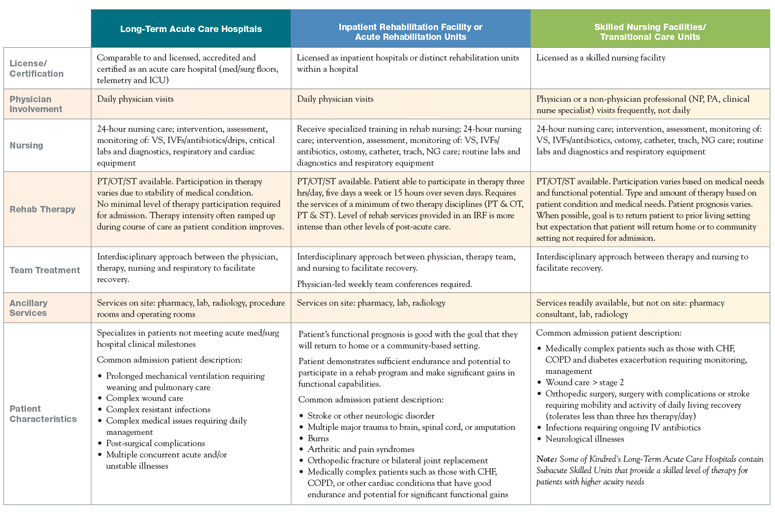
Levels of Care
|
|
Long-Term Acute Care Hospitals |
Inpatient Rehabilitation Facility or Acute Rehabilitation Units |
Skilled Nursing Facilities/Transitional Care Units |
| License/Certification |
Comparable to and licensed, accredited and
certified as an acute care hospital (med/surg floors,
telemetry and ICU) |
Licensed as inpatient hospitals or distinct rehabilitation units
within a hospital |
Licensed as a skilled nursing facility |
| Physician Involvement |
Daily physician visits |
Daily physician visits |
Physician or a non-physician professional (NP, PA, clinical
nurse specialist) visits frequently, not daily |
| Nursing |
24-hour nursing care; assessment, planning,
implementing, evaluating of: VS, IVFs/antibiotics/
drips, critical labs and diagnostics, respiratory and
cardiac equipment, catheter, trach, NG care |
Receive specialized training in rehab nursing; 24-hour nursing
care; intervention, assessment, monitoring of: VS, IVFs/
antibiotics, ostomy, catheter, trach, NG care; routine labs and
diagnostics and respiratory equipment |
24-hour nursing care; intervention, assessment, monitoring of:
VS, IVFs/antibiotics, ostomy, catheter, trach, NG care; routine
labs and diagnostics and respiratory equipment |
| Rehab Therapy |
PT/OT/ST available. Participation in therapy
varies due to stability of medical condition.
No minimal level of therapy participation required
for admission. Therapy intensity often ramped up
during course of care as patient condition improves. |
PT/OT/ST available. All patients able to participate in therapy
three hrs/day, fve days a week or 15 hours over seven days.
Requires the services of a minimum of two therapy disciplines
(PT & OT, PT & ST). Level of rehab services provided in an
IRF is more intense than other levels of post-acute care. |
PT/OT/ST available. Participation varies based on medical needs
and functional potential. Type and amount of therapy based on
patient condition and medical needs. Patient prognosis varies.
When possible, goal is to return patient to prior living setting
but expectation that patient will return home or to community
setting not required for admission. |
| Team Treatment |
Interdisciplinary care approach between physician,
nursing, therapy, respiratory, pharmacy and
nutrition services to facilitate healing and recovery |
Interdisciplinary approach between physician, therapy team,
and nursing to facilitate recovery; physician-led weekly team
conferences required. |
Interdisciplinary approach between therapy and nursing to
facilitate recovery |
| Ancillary Services |
Services on site: pharmacy, lab, radiology,
procedure rooms |
Services on site: pharmacy, lab, radiology |
Services readily available as send outs, but not on site:
pharmacy consultant, lab, radiology |
| Patient Characteristics |
Specializes in patients not meeting acute med/surg
hospital clinical milestones quickly. Patients most
often transition from the intensive or critical care
unit of a short-term hospital for continued, acutelevel care.
Common admission patient description:
- Prolonged mechanical ventilation requiring
weaning and pulmonary care
- Complex wound care
- Multiple resistant infections
- Complex medical issues requiring daily
physician management
- Major post-surgical complications
- Multiple concurrent acute and/or
unstable illnesses
|
Patient’s functional prognosis is good with the goal that they
will return to home or a community-based setting.
Patient demonstrates sufficient endurance and potential to
participate in a rehab program and make significant gains in
functional capabilities.
Common admission patient description:
- Stroke or other neurologic disorder
- Multiple major trauma to brain, spinal cord, or amputation
- Burns
- Arthritic and pain syndromes
- Orthopedic fracture or bilateral joint replacement
- Medically complex patients such as those with CHF, COPD, or other cardiac conditions that have good endurance and potential for significant functional gains
|
Common admission patient description:
- Medically complex patients such as those with CHF,
COPD and diabetes exacerbation requiring monitoring,
management
- Wound care > stage 2
- Orthopedic surgery, surgery with minor complications
or stroke requiring mobility and activity of daily living
recovery (tolerates less than three hrs therapy/day)
- Infections requiring ongoing IV antibiotics
- Neurological illnesses
Note: Some of Kindred’s Transitional Care Hospitals contain
Subacute Skilled Units that provide a skilled level of therapy for
patients with higher acuity needs
|
How Kindred Healthcare Can Help
We specialize in the treatment and rehabilitation of the post-intensive care and complex medical patient requiring continued intensive care, including specialized rehabilitation, in an acute hospital setting.
Our team of skilled and caring clinicians in our long-term acute care hospitals can be the right partner for you for your patients who have been in an ICU, critical care unit or who are chronically ill and readmit to the hospital frequently. We have proven success in treating patients with pulmonary disease and respiratory failure, including a long history of liberating patients from mechanical ventilation and artificial airways.
With daily physician oversight, ICU/CCU-level staffing, 24/7 respiratory coverage and specially trained interdisciplinary teams, we work to improve outcomes, reduce costly readmissions, and help patients transition to a lower level of care.
If you have a critically ill patient in need of care after a hospital stay, call a Kindred Clinical Liaison for a patient assessment. Our experts will help you determine whether an LTAC stay is appropriate for your patient. If you are unsure of who your Kindred representative is, please feel free to contact us and speak with a Registered Nurse who can assist.
References:
- MedPAC 2004; RTI 2012.
- MedPAR 2010
- Doug Irving. Chronic Conditions in America: Price and Prevalence. RAND Corporation. Jul 2017. https://www.rand.org/blog/rand-review/2017/07/chronic-conditions-in-america-price-andprevalence.html
- Hospital Readmissions Reduction Program (HRRP). Centers for Medicare & Medicaid Services. Jan 2019. https://www.cms.gov/medicare/medicare-fee-for-service-payment/acuteinpatientpps/readmissions-reduction-program.html
- Melissa K. Palardy. The Rise of Super SNFs and Their Impact on Long-Term Care. PatientPing. Jan 2018. http://blog.patientping.com/the-rise-of-super-snfs-and-their-impact-on-long-term-carefacilities